This topic takes on average 55 minutes to read.
There are a number of interactive features in this resource:
 Biology
Biology
 Human biology
Human biology
 Science
Science
There are two types of diabetes. Type 1 diabetes which results from autoimmune destruction of certain cells in the pancreas, so the body stops producing the hormone insulin. A combination of genetic and environmental factors are believed to trigger the autoimmune disease. Diet and lifestyle however, have nothing to do with causing this type of diabetes.
Type 2 diabetes occurs when the body is still capable of producing insulin, but the amount produced is not enough to control sugar levels.
In both, the body cannot regulate the level of glucose in the blood. This can be because the body cells do not respond properly to the insulin produced, or because the production of insulin decreases.
Symptoms: develop quickly. Tiredness, excessive urine production, weight loss, increased thirst and blurred vision.
Symptoms: same as for type 1 but less severe and may go undetected for many years.
Type 1 diabetes is an auto-immune disease. The person's immune system attacks the cells in the pancreas that make insulin. These cells are called the islets of Langerhans. The immune system destroys them as if they were an infection. Insulin production is quickly and dramatically stopped.
People with type 1 diabetes often have a particular form of a gene that is involved in the production of cell-recognition proteins. They trigger the immune system to destroy the insulin-producing cells.
It may soon be possible to develop a genetic test to identify people who are at a high risk of developing type 1 diabetes. Furthermore, where there is evidence of a faulty gene, it may even become possible to replace the faulty gene using gene therapy.
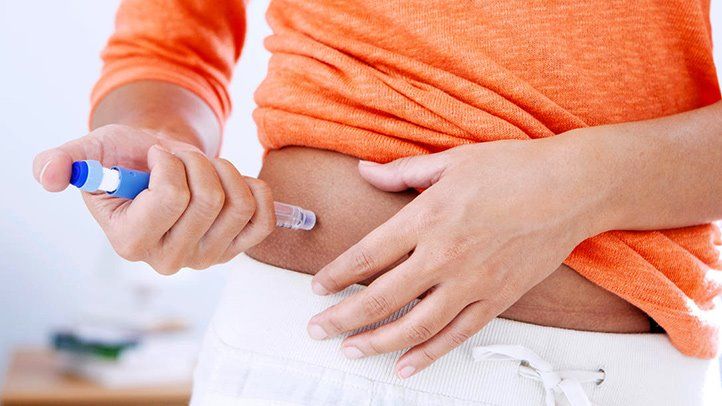
Obesity, and a lack of physical exercise, are linked to an increased likelihood of developing type 2 diabetes. It is more likely to develop if people have a diet that contains lots of saturated fats, sugar and is low in fibre. Some insulin production continues but the liver and body cells do not respond to it normally.