This topic takes on average 55 minutes to read.
There are a number of interactive features in this resource:
 Biology
Biology
 Human biology
Human biology
 PSHE / Citizenship studies
PSHE / Citizenship studies
 Science (applied)
Science (applied)
Human hormones are organic chemicals produced in specialised endocrine glands. They are released directly into the blood stream and are carried to their target organs in the blood. The cells of the target organs have specific receptors for the hormones. Hormones are involved in the coordination and control of many long term processes in the body such as growth and development. They are also involved in some rapid responses - for example controlling the levels of glucose in the blood and the ‘fight-or-flight’ response.
Hormonal diseases usually involve the problems that result when the body lacks a particular hormone or makes too much of one. The treatment will depend on whether the body has too little or too much of a particular hormone, and why.
Diabetes is not a single condition. Diabetes mellitus (or ‘sweet fountain’) is the most common form of diabetes. It involves the hormone insulin and affects the control of sugar levels in the blood. Diabetes insipidus (or ‘watery fountain’) involves the hormone ADH (antidiuretic hormone) and results in the production of large volumes of dilute urine. Again, untreated it can be fatal.
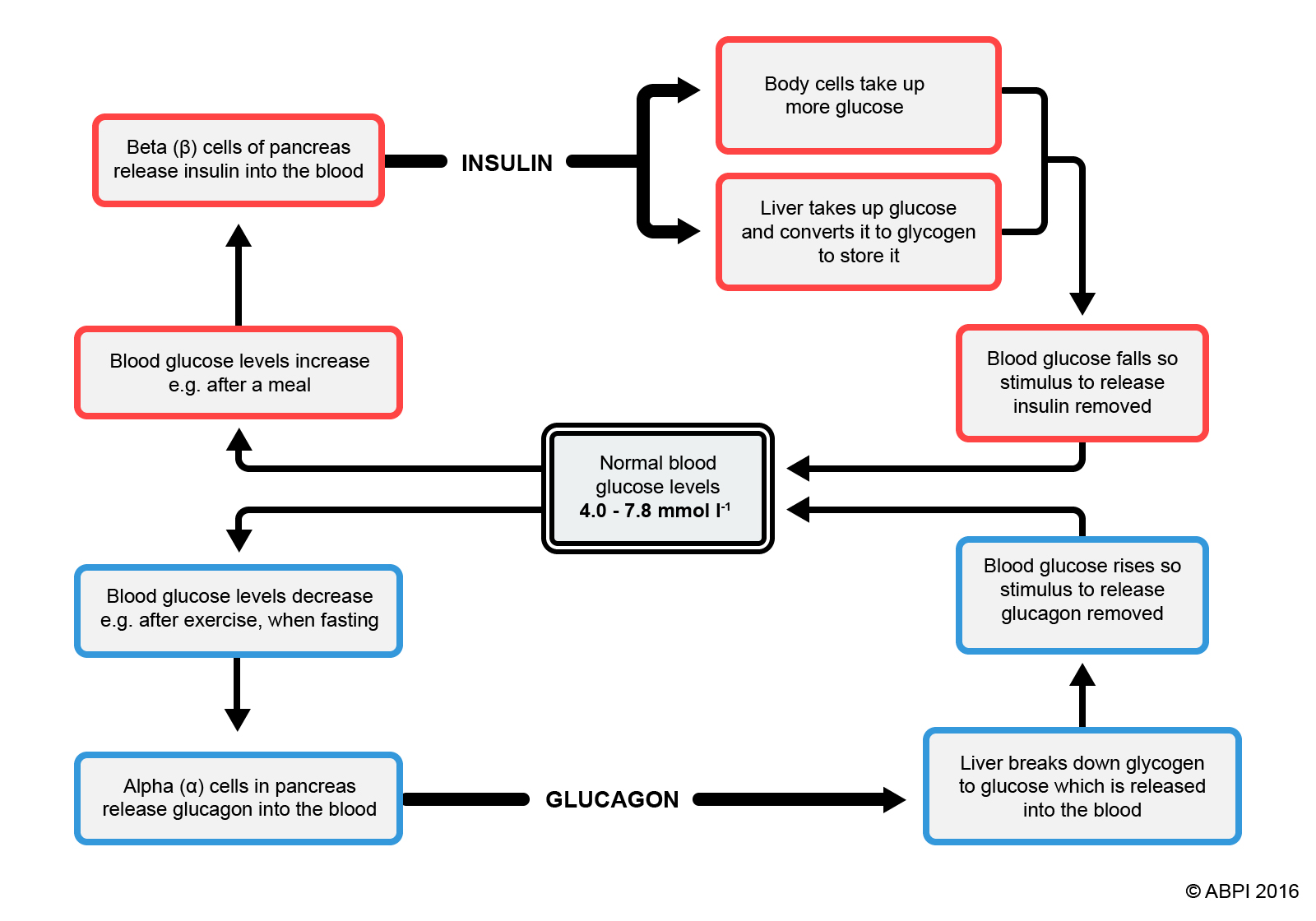
The interaction of the hormones insulin and glucagon are key to the maintenance of the blood sugar levels of the body within normal limits
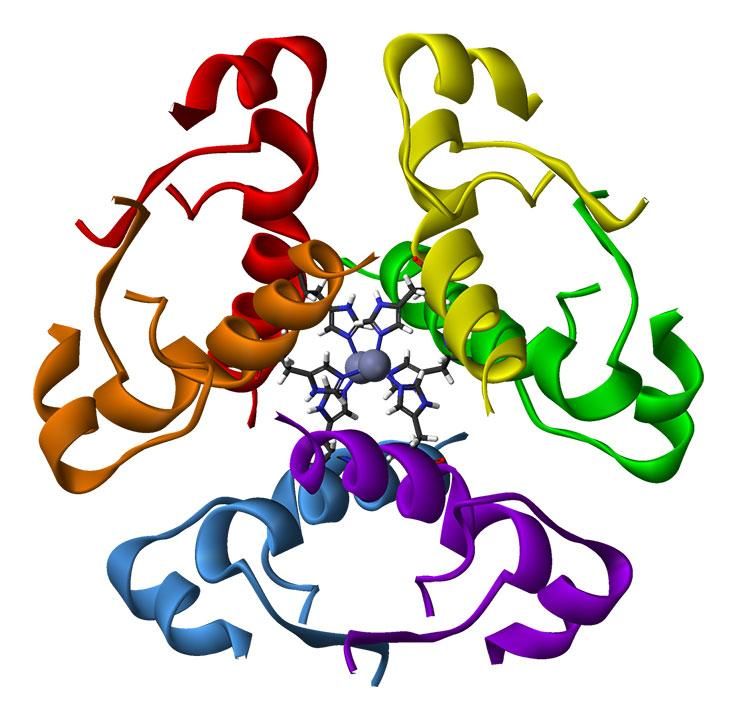
Human insulin produced by genetically modified bacteria has revolutionised treatment for people with diabetes
(Photo credit: Benjah-bmm27, Wikimedia Commons)
In treating diabetes the aim is to replicate, as closely as possible, the normal control of blood sugar levels.
There are two types of diabetes mellitus.
Type 1 diabetes usually affects people from childhood or early adulthood. It occurs when the Islets of Langerhans in the pancreas – the cells that usually produce insulin - fail. Without insulin, control of the blood glucose is lost. Glucose cannot be taken into the cells and so cannot be used in cellular respiration. This results in hyperglycaemia – a rise in the blood glucose levels that causes many problems for the body. Glucose is excreted in the urine. The raised levels of glucose in the blood and lack of glucose in the cells can, if untreated, be fatal. Treatment involves replacing the insulin by regular injections. The challenge for the medical profession is how to replicate the fine control of the natural systems. So far this isn’t possible – but techniques are improving all the time.
Originally the insulin needed was extracted from the pancreases of pigs and other animals slaughtered for meat. This had a number of associated problems – for example
Now genetically modified bacteria are used to produce human insulin. They are cultured in fermenters. The insulin produced is pure human insulin, and the supply of the drug can be tailored to the numbers of people who need it rather than the number of people wanting to eat meat.
It is important to enable people with diabetes to monitor and control their blood glucose as simply and accurately as possible.
|
Finger prick blood tests to measure the blood glucose levels followed by insulin injections.
|
Works well, but requires discipline from the patient. They must take care with their diet, avoiding too much carbohydrate food, check their blood glucose levels regularly, inject insulin a given time before eating and try to maintain a very regular routine. |
|
Insulin pumps have a line into the body and supply short-acting insulin doses through the day.
(Permission for use granted by Jayesh Mirpuri) |
Gives relatively good control. There is more flexibility than with insulin injections. However there is the possibility of infection at the entry site to the body and there are more blood tests because the insulin delivered is very short acting. |
|
Pancreas transplants replace the ineffective pancreas with one that produces insulin from a donor.
(Photo credit: Herecomesdoc, Wikimedia Commons) |
If a transplant works it restores normal function. There are not many pancreases available for transplantation. It requires major surgery and the recipient will need immunosuppressant drugs for life. |
|
Stem cell transplants
(Credit: Nissim Benvenisty) |
The hope is that stem cells will be injected into the pancreas to produce functioning insulin-producing cells. This is still experimental but scientists are hopeful that in the future it may provide a cure for diabetes. |
Type 2 diabetes is rather different. It tends to develop later in life, and it is strongly associated with obesity and lack of physical exercise. The pancreatic cells may produce less insulin than previously, but more often the body cells become less receptive to the effects of insulin.
The first line of treatment is usually for patients to lose weight and become more active – this alone can reverse many of the changes and remove the symptoms of diabetes. Only then will drugs be used.
People affected by diabetes insipidus can pass up to 20 litres of water in 24 hours. Unsurprisingly, they also feel constantly thirsty. In diabetes insipidus, either the hypothalamus of the brain no longer makes the hormone ADH, or the kidney tubules stop responding to ADH. ADH is the hormone needed to make the distal convoluted tubule and the collecting duct of the nephrons in the kidneys permeable to water, so it can be reabsorbed into the blood.
If your diabetes insipidus is caused by a lack of ADH, you may be given the drug desmopressin which has a similar effect on the kidneys as ADH and allows your body to conserve water. You may be given thiazide diuretics that concentrate the urine and so reduce the amount of water lost. NSAIDs or non-steroidal anti-inflammatory drugs such as ibuprofen also seem to help reduce the volume of urine produced – though scientists are not sure why!
If your kidney tubules do not respond to ADH, you may also be prescribed thiazide diuretics and NSAIDS, because they act on different mechanisms to conserve water and reduce the volume of urine produced.
More detailed information about the causes and treatment of diabetes can be found here.
There are many endocrine glands in the body. Common problems include: